The survival and recovery of critically injured or ill victims depends on—
Recognition and response by the lay responder.
Early activation of the EMS system.
Professional rescuer care.
Prehospital care provided by advanced medical personnel.
Hospital care.
Rehabilitation.
The Cardiac Chain of Survival
- • Early recognition of the emergency and early access to EMS
• Early cardiopulmonary resuscitation (CPR)
• Early defibrillation
• Early advanced medical care
Steps to follow in an emergency:
Size up the scene.
determine is scene is safe, put on your PPEs (personal protective equipment), try to find out what happened, determine the number of victims and what additional help may be needed
Perform an initial assessment to identify life-threatening conditions.
check the victim for:
- Consciousness
Signs of life (movement and breathing)
Pulse
Severe bleeding
Summon advanced medical personnel.
If you are sure the victim needs additional help, or if you are unsure of the victim’s condition or you notice the condition worsening, call 9-1-1 or the local emergency number
Obtain Consent Before Providing Care to a conscious victim
- Identify yourself
State level of training
Ask if you can help
Explain that you would like to assess him or her to find out what is wrong
and/or tell the victim what is wrong and explain what first aid you want to do
![]()
Benefits of using a resuscitation mask:
- The possibility of disease transmission is reduced.
A seal is created over both the victim’s mouth and nose.
Air can be delivered to the victim more quickly through both the mouth and nose.
The device can be connected to emergency oxygen if it has an oxygen inlet, thus increasing the oxygen concentration the victim receives up to 100%.
Signs and symptoms of respiratory distress:
- Slow or rapid breathing
Unusually deep or shallow breathing
Shortness of breath or noisy breathing
Dizziness, drowsiness or light-headedness
Changes in the level of consciousness
Increased heart rate
Chest pain or discomfort
Flushed, pale, ashen or bluish skin
Unusually moist or cool skin
Gasping for breath
Wheezing, gurgling or high-pitched noises
Inability to speak in full sentences
Tingling in hands, feet or lips
Care for Respiratory Distress
- Summon more advanced medical personnel
Have victim rest in comfortable position that makes breathing easier
Reassure and comfort the victim
Keep victim from getting chilled or overheated
Assist victim with any of his or her prescribed medications
Give emergency oxygen, if it is available and you are trained to do so
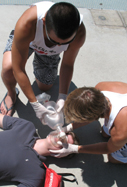 A BVM (bag valve mask) reduces the risk of disease transmission and increases the level of oxygen being delivered to a victim. Rescue breathing only gives a victim about 16% oxygen, a BVM can deliver 21%
A BVM (bag valve mask) reduces the risk of disease transmission and increases the level of oxygen being delivered to a victim. Rescue breathing only gives a victim about 16% oxygen, a BVM can deliver 21%
Steps to use a BVM
- • Rescuer 1 performs an initial assessment while Rescuer 2 assembles the BVM.
• Rescuer 1 seals the mask and opens the airway.
• Rescue 2 begins ventilations.
• Look for movement and recheck for breathing and a pulse about every 2 minutes.
Signs and Symptoms of a Heart Attack
- Persistent chest discomfort, pain or pressure that lasts longer than 3 to 5 minutes, or goes away and comes back.
Discomfort, pain or pressure in either arm, back or stomach.
Chest discomfort, pain or pressure that spreads to the shoulder, neck, jaw or arms.
Shortness of breath or trouble breathing.
Nausea or vomiting.
Dizziness, light-headedness, loss of consciousness or fainting.
Pale, ashen, grayish or bluish skin.
Sweating—face may be moist or person may be sweating profusely.
Denial of signs or symptoms.
Care for a Heart Attack
- Immediately summon advanced medical personnel.
Have the victim stop what he or she is doing and rest.
Loosen any tight or uncomfortable clothing.
Closely monitor the victim until advanced medical personnel arrive.
Notice any changes in the victim’s appearance or behavior.
Comfort the victim.
If medically appropriate and local protocols or medical direction permit, give aspirin if the victim can swallow and has no known contraindications. Never delay calling 9-1-1 to do this.
Assist the victim with his or her prescribed medication
Give emergency oxygen, if it is available and you are trained to do so.
Be prepared to give CPR or use an AED
Signs and symptoms of cardiac arrest (a life-threatening emergency):
- Unconsciousness
No movement or breathing
No pulse

continue CPR until:
- another trainer rescuer arrives and takes over
an AED is available and ready to use
you are too exhausted to continue
the scene becomes unsafe
you notice an obvious sign of life
The Heart
Right atrium – receives blood from body
Left atrium – receives blood from lungs
Right ventricle – pumps blood to lungs
Left ventricle – pumps blood to body
__________________________________________
Causes of Cardiac Arrest
coronary heart disease
ventricular tachycardia
ventricular fibrillation
bradycardia (extreme slowing of the heart)
respiratory arrest
electrocution
drowning
choking
trauma
from EMS World:
“Commotio cordis, also known as cardiac concussion, occurs when a person receives a blow to the chest during a vulnerable window during diastole of the heart. This concussive force, occurring during the upstroke of the T-wave, triggers ventricular fibrillation Sudden Cardiac Arrest. Commotio cordis can occur in both contact and noncontact sports and should be suspected anytime an athlete experiences blunt trauma to the chest followed by sudden collapse.”
__________________________________________
Normal breathing is regular, quiet and effortless. Agonal breathing is a gasping noise that many people make when they collapse from cardiac arrest. It can be mistaken for breathing. But an isolated gasp or gurgle (in the absence of other breathing) is not normal breathing.
In the International Liaison Committee on Resuscitation 2005 Consensus on ECC & CPR Science and Treatment Recommendations we read that agonal gasps are common in the early stages of cardiac arrest. Bystanders often report to dispatchers that victims of cardiac arrest are ‘breathing’ when they demonstrate agonal gasps; this can result in the withholding of CPR from victims who might benefit from it.
__________________________________________
It is possible to receive a mild shock if an implantable ICD delivers a shock to the person during CPR. The risk to responders is minimal because the amount of electrical energy involved is low.
__________________________________________
__________________________________
In a life-threatening emergency, doing something right is better than doing nothing at all.
When a rescuer is unable, untrained or unwilling to perform full CPR, continuous Compression Only CPR or Hands-only CPR for witnessed sudden collapse, can be effective in caring for a person with no signs of life.
Hands only CPR (Yes, a professional rescuer would use their higher level of training.)
The Red Cross has produced a video for people who have not been trained in CPR or who are not sure what to do.
http://www.youtube.com/watch?v=m71yc5m8V38
Elements of Quality Adult CPR Compressions
Keeping arms as straight as possible
Positioning the shoulders directly over hands
Compressing the chest at least 2 inches
Compressing at least 100 times per minute
Letting the chest rise completely before pushing down again
__________________________________
– – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – –
39% of European countries require CPR training
for a driving license. The European Resuscitation Council (ERC) and European Driving Schools Association (EFA are working towards mandatory CPR training for new drivers across Europe. (“Learn to Drive. Learn CPR.”,) The European Parliament has backed mandatory CPR training in its new Driving License Directive proposal.
“Cardiac arrest is a major health problem in Europe and around the world. Every year over 400,000 people in Europe and 60,000 in Italy are affected by cardiac arrest. In 70% of cases, cardiac arrest is seen by laypeople who could start cardiopulmonary resuscitation (CPR) if they knew how to do it.
The immediate initiation of CPR can double or triple survival from cardiac arrest. In fact, if witnesses of cardiac arrest start CPR before the ambulance arrives, the victims’ chances of survival increase two to three times compared to cases in which CPR is not started.”
The above was as of early 2025. See https://cprguidelines.eu/news for updates.
– – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – –
CERP is not a different way of doing CPR, it refers to a Cardiac Emergency Response Plan (CERP), for example in a school.
Citizen CPR is not a different way of doing CPR, it has been described as “a system of care involving the entire community . . . fostering a culture of preparedness and response within communities.”
– – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – –
see also:
AED quick facts includes basic steps of how to use an AED
In anticipation of taking a CPR certification class, please see: How to pass a Red Cross written test for advice.
Bloodborne Pathogens quick facts
__________________________________
The author of this webpage, (written as a homework reading assignment for my students), does not give any warranty, expressed or implied, nor assume any legal liability or responsibility for the accuracy, completeness, or usefulness of any information, product, or process included in this website or at websites linked to or from it. Users of information from this website assume all liability arising from such use.
Note to on-line users not in my classes: this is a study sheet. It is not complete instruction in CPR or the topic named in the webpage title. This webpage is not complete training and will not substitute for a class, especially not for a CPR certification class.