Hands only CPR is a cardiopulmonary resuscitation class
designed to teach bystanders how to perform hands-only CPR if they witness the sudden collapse of a teen or an adult.
The American Red Cross and the American Heart Association (AHA) teach the same steps for giving hands-only CPR. (cardiopulmonary resuscitation). These two organizations stress different parts. For my classes I like to include both, so both are mentioned at this webpage.
The Red Cross says; “If you are not trained in full CPR, Hands-only CPR is CPR without rescue breaths which is simple to learn and easy to remember, especially outside medical settings. It increases the likelihood of surviving cardiac arrest, when the heart stops beating or beats too ineffectively to circulate blood to the brain and other vital organs.
The American Heart Association answers the question:
Why learn hands-only CPR?
Cardiac arrest – an electrical malfunction in the heart that causes an irregular heartbeat (arrhythmia) and disrupts the flow of blood to the brain, lungs and other organs – is a leading cause of death. Each year, more than 350,000 EMS-assessed out-of-hospital cardiac arrests occur in the United States.
When a person has a cardiac arrest, survival depends on immediately receiving CPR from someone nearby.
According to the American Heart Association, about 90 percent of people who suffer out-of-hospital cardiac arrests die.
CPR, especially if performed immediately, can double or triple a cardiac arrest victim’s chance of survival”
________________________________________
Cardiac arrest is a life-threatening emergency when a person’s heart stops beating. They will also stop breathing at the same time. Often it is the first sign of heart trouble.
Cardiac arrest is the leading cause of death in the United States, every year killing more people than cancer, stroke, lung disease, accidents, firearms, or diabetes. Cardiac arrest affects people of all ages, even teens, twenty somethings and the very young.
Most cardiac arrests happen away from a hospital where care needed to correct the condition is not readily available. If more people are trained to at least recognize the emergency, call for professional help (call 911 or the local emergency number), and do hands only CPR, more cardiac arrest victims can be saved.
Heart attacks are the leading cause of death for men and women when they lead to cardiac arrest. Almost half of the people who have heart attacks die from them. Medications to treat a heart attack and limit the damage from a heart attack must be given as soon as possible.
A heart attack can happen before cardiac arrest, or the heart attack and cardiac arrest can be sudden and happen at the same time. Not all heart attacks lead directly to cardiac arrest and some heart attack victims do not notice a mild heart attack (or might not notice even more than one mild heart attack).
A heart attack victim might or might not have a lot of pain; extreme weakness or tiredness might be the main symptoms. Symptoms might start out slowly or come and go.
Signs and symptoms of a heart attack include:
Persistent chest discomfort, pain or pressure that lasts longer than 3 to 5 minutes, or goes away and comes back, or persists even during rest.
Discomfort, pain or pressure in either arm, back or stomach.
Chest discomfort, pain or pressure that spreads to the shoulder, back, neck, jaw or arms.
The pain is sometimes described as a feeling of fullness, squeezing, aching or heaviness in the chest that can be mild or strong.
Shortness of breath or trouble breathing that can start before pain or along with the chest discomfort or even without the chest discomfort.
Nausea (feeling sick to your stomach) or vomiting.
Dizziness, light-headedness, loss of consciousness or fainting.
Pale, ashen, grayish or bluish skin, especially around the face.
Sweating—face may be moist or person may be sweating profusely. It is sometimes described as breaking out in a cold sweat.
Unexplained fatigue (tiredness) or lightheadedness.
Denial of signs or symptoms. Denial can happen even when the victim is in extreme pain. For example, you might notice a family member who looks very uncomfortable, who is pale and sweating. When you ask them how they are doing you notice that they are having trouble breathing but they say it’s only a little indigestion/the flu/normal aging. If you suspect a heart attack is happening, even if they insist that you should not call 911, you should call.
________________________________________
A person who is fully oriented to their surroundings is conscious. People can be partially conscious, for example, if they hit their head they might not know what happened to them but might know who they are and where they are. Conscious or partially conscious people do not need CPR compressions.
Fainting is loss of consciousness caused by a temporary, often sudden, lack of oxygen to the brain. Example: stood up too fast after prolonged sitting or lying down (more likely for pregnant, elderly), or after a large meal (especially with alcohol). Fainting usually corrects itself when people collapse, since blood flow to their brain increases when they become horizontal and their head is at the same level as their heart.
Being asleep is not the same as being unconscious (not conscious). Someone who is sleeping will wake up when you tap them on the shoulder and/or speak loudly to them, someone who is unconscious will not respond.
You do not have to get consent (permission) from an unconscious victim to help them. But there are rules you will learn in a first aid class about how you should not force first aid on a conscious, sane, sober adult who doesn’t want it, even if they really need it. (But you can and should call 911 for them if they really need help, even if they don’t want you to. Example: a heart attack victim who is in denial that it is a heart attack.)
________________________________________
________________________________________
Your first step when you witness a teen or adult suddenly collapse will be to check the scene for safety to be sure it is safe for you to approach them. For example, if a person walks out of a chemical storage area coughing and suddenly collapses, you could be affected by the same chemical leak if you get too close too quickly. Do not risk becoming a victim yourself. Stop briefly and be sure it is safe for you to approach the victim.
(Details about your quick evaluation of scene safety are at: Checking the Scene for Safety.)
If you have disposable (not latex, nitrile preferred) gloves you should put them on, but should not take time to go looking for them.
If it is safe to approach the victim, check the victim to determine if the victim is conscious or not. Tap them on the shoulder, shout at them (use their name if you know it) and tap again to see if they are okay. Look for signs of rhythmic, normal breathing, which can be as simple as noticing if their chest is rising and falling from breaths they inhale/exhale.
(Normal breathing is regular, quiet and effortless. Agonal gasps are common in the early stages of cardiac arrest. Bystanders often report to 911 dispatchers that victims of cardiac arrest are ‘breathing’ when they have agonal gasps, as a result CPR is not given to victims who might benefit from it. (Sometimes people mistakenly think a victim of cardiac arrest had a seizure instead because they seem to be breathing.) An irregular, gasping or shallow breath is not normal breathing and should be cared for as if the person is not breathing at all.)
(If the person is face down, determine if the victim is conscious or not and if they are unconscious (not conscious), carefully but quickly roll them over, (unless you have reason to suspect a spinal injury, then do what you are taught in a first aid or lifeguard class), protecting their head, and then quickly look for normal breathing.)
If they do not respond when you tap and yell, call 911, (or have a bystander call),
Details about calling 911, including why and when to call, teaching children to call, tips for making wireless 911 Calls, times NOT to call 911 and more are at How to Call 911.
and if they are not breathing, start chest compressions.
(If an AED is not nearby, start CPR and send someone who knows where one is to get it. If you use the AED you still need to have called 911.)

________________________________________
Elements of Effective, Quality CPR Compressions
– For chest compressions to be effective, they must be performed on a firm, flat surface. (For example, a victim who collapsed on stairs would need to be moved.)
Kneel beside the person. Your knees should be near the person’s body and spread about shoulder width apart.
Place the heel of one hand in the center of their chest, with your other hand on top.
Interlace your fingers and make sure they are up off the chest.
Use the heel of the hand, not your palm, to give compressions to a child or adult.
– – – If you could see through to the rib cage, this is what it would look like where you correctly place
your hand on the center of the chest, but not as low as the abdomen (belly/stomach area):
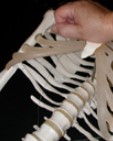
– Keep your arms as straight as possible ( you can lock your elbows to keep your arms straight
– Position your body so that your shoulders are directly over your hands
The photo below shows the wrong way, arms out at an angle (shoulders NOT directly over hands), and the heel of the hand not quite on the center of the chest:
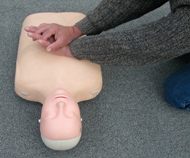
– Compress the chest at least 2 inches deep
– Compress at least 100 times per minute
– Let the chest rise completely before pushing down again
________________________________________
Continue CPR chest compressions until:
– an AED is ready to use (as soon as it arrives turn it on and do what it says to do). If possible, have one person continue compressions while another sets up the AED.
– the scene becomes unsafe (examples: fire is moving through a building towards you, rising floodwater or aftershocks from an earthquake that are making the building unstable)
– you notice an obvious sign of life, such as normal breathing
– EMS personnel (fire, EMT, paramedic) arrive and take over
(Don’t stop when you hear the ambulance or fire truck sirens, it will still take a few more minutes for help to get to where you are. Don’t stop when the EMT comes on scene, they might want you to continue compressions while they unpack their gear.)
– you are too exhausted to continue
If you become tired realize that since you either called 911 or had someone else call, help is on the way.
Concentrate on pushing hard and fast.
– – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – –
39% of European countries require CPR training
for a driving license.
The European Resuscitation Council (ERC)
and European Driving Schools Association (EFA)
are working towards mandatory CPR training for new drivers across Europe.
(“Learn to Drive. Learn CPR.”)
The European Parliament has backed mandatory CPR training in its new Driving License Directive proposal.
“Cardiac arrest is a major health problem in Europe and around the world. Every year over 400,000 people in Europe and 60,000 in Italy are affected by cardiac arrest. In 70% of cases, cardiac arrest is seen by laypeople who could start cardiopulmonary resuscitation (CPR) if they knew how to do it.
The immediate initiation of CPR can double or triple survival from cardiac arrest. In fact, if witnesses of cardiac arrest start CPR before the ambulance arrives, the victims’ chances of survival increase two to three times compared to cases in which CPR is not started.”
The above was as of early 2025. See https://cprguidelines.eu/news for updates.
– – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – –
The European Resuscitation Council
also recognizes the importance of hands only CPR and estimates using it could save at least 100,000 more lives in Europe alone each year. “Push fast and firmly, and start immediately… Everyone, including children, can do this. This simple procedure is safe and markedly increases the victim’s chance of survival.”
European Resuscitation Council training materials include this last step in CPR:
SMILE
•
Once the emergency services arrive, continue until you are told to stop
•
Smile! Your hands could restart a heart and save a life
•
Doing something is ALWAYS better than doing nothing
•
Well done!

The British Heart Foundation
is also promoting hands only CPR. “At the moment less than 10 percent of the 30,000 people in the United Kingdom who have a cardiac arrest out of hospital each year survive long enough to leave hospital alive. If someone carries out early CPR, it may double a casualty’s chances of survival. Hands-only CPR should increase the number of bystander interventions and save lives.”
________________________________________
________________________________________
From The Olympian (Olympia, Wash.) as quoted in EMSWORLD, “. . . One of the most challenging things for us is to get citizens to engage in CPR before we arrive, said Karen Weiss, a Lacey, Washington Fire paramedic. “It can be really scary, people are hesitant, they’re fearful they’re going to harm somebody.”
But, it’s vital, Weiss said. Performing CPR increases the survival rate for cardiac arrest victims by about 50 percent. Because more than 80 percent of heart attacks in Thurston County happen outside of a hospital, defibrillators aren’t always handy. CPR helps them work better once medics arrive on scene, she explained.
“Don’t stop until we get there,” Weiss said. “Because we’re sending you the closest EMS unit to you, and they’ll take over when they arrive.”
______________________________________________________
To a large extent, heart disease is preventable.
You might be at risk of a heart attack if you:
- have uncontrolled high blood pressure
- have high cholesterol
- are overweight or obese
- are diabetic
- are not active
- smoke (one year after you quit smoking your risk of coronary heart disease is cut in half)
- are subject to breathing second hand smoke
- have a family history of heart disease, and/or a family history of unexplained deaths before the age of 50
- have experienced sudden and unexplained fainting and/or chest pain during physical exertion/exercise.
- use recreational drugs, especially amphetamines/stimulants and cocaine, and especially if the drugs had added toxic substances such as talc, herbicides, or poisons
- engage in sweating routines for weight loss and/or have eating disorders causing electrolyte imbalances
Your doctor might advise cardiac screening with an echocardiogram (ECG) when you report some of the above.
Are non-professionals any good at doing CPR?
In a July 2018 article in Resuscitation on Analysis of bystander CPR quality during out-of-hospital cardiac arrest . . .
https://www.resuscitationjournal.com/article/S0300-9572(18)30223-5/fulltext?showall=true=
“We found that bystanders perform high-quality CPR, with strong adherence rates to existing Resuscitation Guidelines.”
Optional reading, or just scroll through, to get ready for a CPR class: CPR manikin use
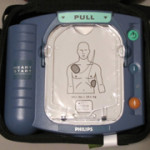
An automated external defibrillator (AED) is a small computer that analyzes a victim’s heart rhythm and if necessary, tells you to deliver a lifesaving shock to a victim of sudden cardiac arrest.
When you turn it on it talks to you and tells you the steps to use it.
Most models even have a map on the pads you place on the victim’s chest showing you where to put them:

An AED won’t shock someone who does not need it.
You do not need a certification to use an AED or give CPR
Take a look at photos of
AED locations at De Anza College
and, if you want to
find out the locations of campus AEDs nearest your classrooms/workplaces.
AED quick facts includes basic instructions for using more than one model of AED (both models we have at De Anza College).
.
________________________________________
A patient who is near the end of life, or has a severe illness that is not expected to be cured or get any better, for example terminally ill with widespread cancer, can consult with their doctor and ask that a
do not resuscitate (DNR) order be written by the doctor.
They then will not be given CPR nor will an AED be used on them.
This formal document is most likely to be found for a patient in a nursing home on their medical record.
A tattoo or t-shirt that says DNR or even “do not resuscitate”
is NOT to be taken as a doctor’s do-not-resuscitate order.
In anticipation of taking a CPR certification class, please see: How to pass a Red Cross written test for advice.
Do it yourself earthquake preparedness
earthquake home hazards survey
A family (and babysitters, caregivers, overnight guests) disaster plan is at:


![]() What to put in a First Aid Kit
What to put in a First Aid Kit
– – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – – –
see also:
Times to suspect a spinal injury (symptoms, causes, signs of spinal injury)
Bloodborne Pathogens quick facts
first aid Secondary Assessment
causes of fainting, altered mental status, sudden altered mental status, unconsciousness
Seizures, causes of and basic care for
Concussion signs and symptoms, prevention
The author of this webpage, (written as a homework reading assignment for my students), does not give any warranty, expressed or implied, nor assume any legal liability or responsibility for the accuracy, completeness, or usefulness of any information, product, or process included in this website or at websites linked to or from it. Users of information from this website assume all liability arising from such use.
Note to on-line users not in my classes: this is a study sheet. It is not complete instruction in CPR or the topic named in the webpage title. This webpage is not complete training and will not substitute for a class, especially not for a CPR certification class.
https://www.metronomeonline.com/